WHITE PAPER
Do You Have eVoucher And Denial Conversion Services That Help To Recoup Your Pharmacy Medication Costs?

Introduction
Copay coupons are an increasingly important way for drug manufacturers to help patients manage out-of-pocket prescription drugs costs. By using a coupon, a patient can access a medication prescribed by their doctor that might otherwise be unaffordable. A February 2022 report by the National Bureau of Economic Research (NBER) noted that coupons have “become nearly ubiquitous” for high-priced brand
name drugs. This statement is supported by a Health Affairs analysis, which found that in 2009 copayment coupons were available for less than 100 brand name drugs. By 2015, that number had increased to more than 700 drugs, and in 2016, 20 percent of “brand prescriptions in commercial insurance plans were filled using some kind of copay assistance option.”
According to a white paper by researchers at the University of Southern California’s Schaeffer Center for Health Policy & Economics, this access is “particularly important given the high cost-sharing imposed on some drugs and increasing deductibles.”
The net impact has been felt by patients across the country, who find themselves faced with increasingly high out-of-pocket costs. Research by IQVIA found patient out-of-pocket costs increased by $4 billion during 2021, reaching a record $79 billion.
Manufacturer-sponsored coupons, along with other assistance options including denial conversion services help patients reduce and manage these costs. Coupons reduce or eliminate copays, while denial conversion covers medications rejected by payers by converting denials into paid claims.
According to IQVIA, $12 billion in coupons were offered to “commercially insured” patients during 2021. The $12 billion figure includes pre-paid debit cards issued to eligible patients by manufacturers. Important to note, enrollees in federal-and-statefunded Medicare and Medicaid programs are not eligible to take advantage of co-pay coupons.
Technology now makes coupons and denial conversion processing instantaneous. PrimeRx automation allows pharmacies to apply savings at the point of the sale with no extra steps.
PrimeRx eVoucher and Denial Conversion allow pharmacies to access both services seamlessly within the PrimeRx operating system. Records are automatically updated and stored.
Voucher and Denial Conversion offer clear benefits to both patients and pharmacies that include:
Reduced patient out-of-pocket costs, which means increased medication adherence.
Increased first fill and refill rates for high-cost medications.
Reimbursement plus payment of an administrative fee for medications filled via a denial conversion program.
Decreased rates of high-cost prescription drug abandonment.
Automated workflows that eliminate the need for additional claims submissions.
Improved patient satisfaction and loyalty
This discussion outlines the specific attributes of PrimeRx eVoucher and Denial Conversion services and how pharmacies can help patients manage costs while improving revenue and workflow efficiency.
The PrimeRx eVoucher with Denial Conversion Solution

The PrimeRx management system includes integrated eVoucher and Denial Conversion Services. PrimeRx offers denial conversion directly, reimbursing pharmacies for medications rejected by payers, and pays a $2.00 per-transactions administrative fee.
Following is an overview of PrimeRx eVoucher and Denial Conversion Services capabilities.
What Are eVoucher Services?
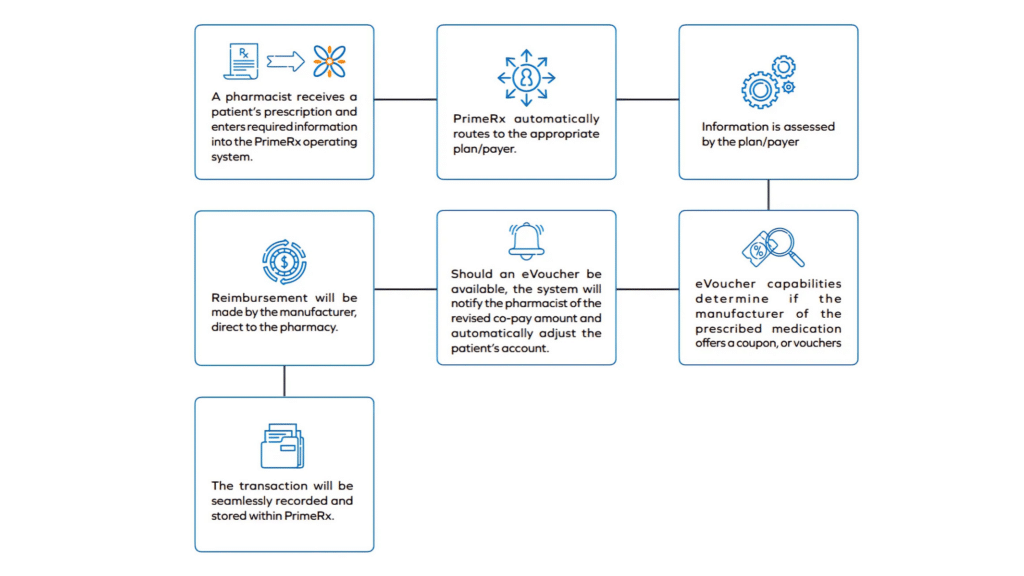
- A pharmacist receives a patient’s prescription and enters required information into the PrimeRx operating system.
- PrimeRx automatically routes patient and prescription information to the appropriate plan/payer. Information is assessed by the plan/payer and returned to the pharmacy via PrimeRx on issues including formulary coverage, patient co-pay amounts, prior authorization requirements, and any step therapy protocols.
- At the same time though, eVoucher capabilities determine if the manufacturer of the prescribed medication offers a coupon, or vouchers, to help reduce or eliminate
the patient’s out-of-pocket costs. - Should an eVoucher be available, the system will notify the pharmacist of the revised co-pay amount and automatically adjust the patient’s account.
- Reimbursement will be made by the manufacturer, direct to the pharmacy.
- The transaction will be seamlessly recorded and stored within PrimeRx. This includes updates to the patient’s record, as well as to the pharmacy’s business accounts.
Denial Conversion Services
The PrimeRx Denial Conversion program is available exclusively to PrimeRx pharmacies.
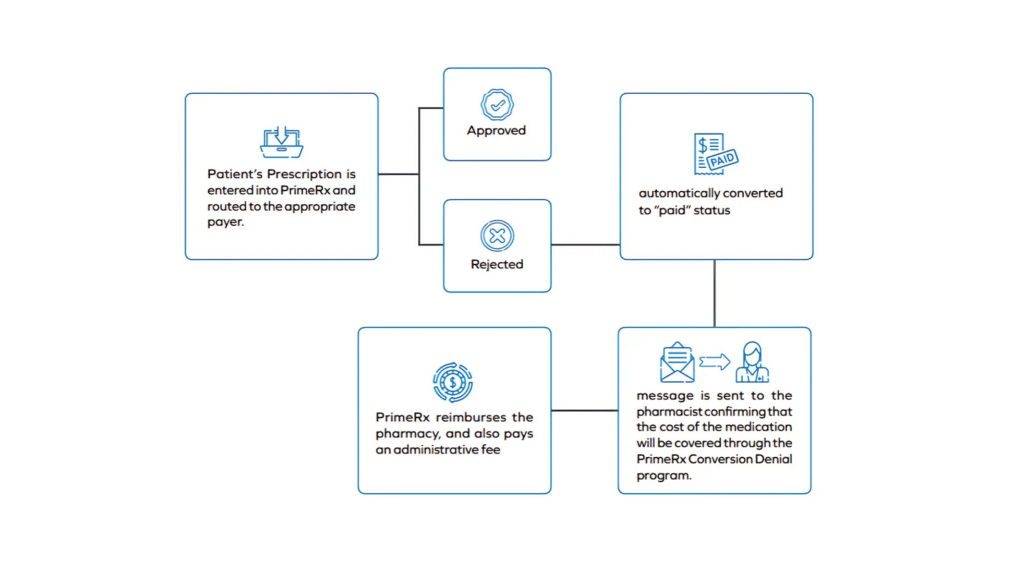
- Similar to the process for eVoucher services, a patient’s prescription is entered into PrimeRx and routed to the appropriate payer.
- Should the claim be rejected by the payer as “non reimbursable for a detected drug or medical device,” the PrimeRx denial conversion solution will intervene.
- The rejected claim is automatically converted to “paid” status, and a message is sent to the pharmacist confirming that the cost of the medication will be covered through the PrimeRx Conversion Denial program.
- PrimeRx reimburses the pharmacy, and also pays an administrative fee, as follows:
- For each denial transaction, the pharmacy is paid a sum that equals the Wholesale Acquisition Cost (WAC) plus 7.5%, less the patient responsibility amount.
- The pharmacy is paid a $2.00 administrative fee for each denial conversion transaction. This fee is intended to offset the pharmacy’s administrative and processing costs.
- Payments will be made by PrimeRx at the end of the month in which the transaction occurred. Denial conversion-related payments will be reconciled against any pending PrimeRx invoices, with the balance posted to the pharmacy’s bank account.
- The pharmacy will receive an electronic notification when a reimbursement has been made.
How Do You Prepare Your Pharmacy for Conversion Denial Reimbursements?
Before a pharmacy can receive reimbursements for medications dispensed through the Denial Conversion Program, a few quick steps are necessary that include:

A Win-Win for Pharmacists and Patients
eVoucher and denial conversion services provide clear benefits. Patients reduce expenses, access preferred medications, and maintain adherence. Pharmacies improve service, increase revenue, and streamline workflows. A more detailed overview of benefits includes:
What Are The Pharmacy Benefits?
- The process is automatic. Every prescription submitted via PrimeRx is automatically assessed for eVoucher availability and denial conversion applicability. There are no additional steps required by the pharmacist.
- The process is seamless. Because the PrimeRx eVoucher and Denial Conversion Services solution kicks in automatically, pharmacist workflows can continue
uninterrupted. This adds efficiency to the pharmacist’s day and helps minimize the risk of errors that can result from distractions and interruptions. - Direct integration within PrimeRx. PrimeRx eVoucher and Denial Conversion Services is included with the PrimeRx operating system, and accessible from the homepage. No need for the pharmacist to access a separate program or jump
between multiple screens. Equally important, all records are seamlessly stored within PrimeRx for easy accessibility and comprehensive records management. - Automated reimbursements require no additional steps by the pharmacy.
- Redeemed eVouchers are automatically submitted to the drug manufacturer and processed for direct reimbursement to the pharmacy.
- PrimeRx automatically notifies the pharmacy about pending denial conversion payments. At the end of each month, PrimeRx issues a direct payment to the pharmacy that reflects the sum total of denial
conversion reimbursements and administrative fees, after reconciliation with any other outstanding PrimeRx invoices. - Increased revenue opportunities. Since cost is regularly cited as a key reason for both medication non-adherence and prescription abandonment, pharmacists can expect improvement in each area, as patients have better access to their medications. This is evidenced by 2021 IQVIA research, which set forth a “rule,” that simply states: “The more a patient is asked to pay, the less likely they are to do so.”
In its research, IQVIA determined that although abandonment rates overall increased by 27 percent during the 2016-2020 period, increases were especially high when co-pays exceeded $50 (21 percent increase in abandonment) and $125 (30 percent increase). By reducing – and in some cases eliminating – patient copay amounts, eVouchers and denial conversion services improve access to medications, which in turn results in increased revenue opportunities for pharmacies.
What Are The Patient Benefits?
- Reduced out-of-pocket costs. Patients recognize immediate cost savings on their medications. In many instances, this means the patient can leave the pharmacy with medication that might have been cost-prohibitive without the copay assistance.
- Access to preferred medications. Patients can obtain exact medications prescribed by their doctors, rather than alternatives approved by their insurance payer. In many instances patients are forced to “settle” for alternative medications that are not as effective, or that generate unpleasant side effects. The PrimeRx solution allows patients to have access to their first-choice medications, in accordance with their prescriber’s expertise.
- Hassle-free pharmacy experiences. Patients no longer need to dread negative experiences at the pharmacy counter. A patient can have confidence they will receive their medication, without any prolonged negotiation with an insurance company, and without having to endure a lengthy claims and appeals process.
- Improved adherence and healthier outcomes. As affordability becomes less of an obstacle, patients will be more likely to adhere to their medication regimes. This in turn will increase the likelihood of improvement in a diagnosed medical condition and prevent a treatable condition from requiring elevated levels of care.
Industry Update: Opposition Manufacturer Copay Coupons

Any discussion about co-payment coupons must acknowledge their critics, including PBMs, payers, lawmakers, and policy analysts. Opponents argue coupons steer patients toward higher-cost brand-name drugs, shift expenses to health plans, and ultimately contribute to higher premiums, according to the National Conference of State Legislatures (NCSL).
These concerns have led to bans on coupons in Medicare and Medicaid, as well as state restrictions, such as prohibiting coupons when generics are available or requiring coupon value to count toward a patient’s out-of-pocket maximum.
But, as researchers from the University of Southern California’s Schaeffer Center for Health Policy & Economics determined, “much remains unsettled” about how coupons affect patient behavior and drug costs. In their analysis, the researchers cite important benefits coupons can have in helping patients access drugs for which there are “imperfect therapeutic substitutes.” While some patients might see little difference in outcomes by using a different drug than the one prescribed by their doctor, others might suffer serious consequences. As the researchers explain, “…substitution may not be suitable due to specific comorbidities, drug interactions, or other individual circumstances. In these cases, coupons help patients afford the therapy chosen by their doctor rather than the one preferred by their PBM.”
Conclusion
For many patients, coupons and denial conversion services provide a lifeline to desperately needed medications. Consider, as an example, the experience detailed by PEW Stateline of one 25-year-old California resident who, after having suffered from debilitating migraines since the age of 12, was finally able to get relief when the first migraine-specific medication became available. That relief was short lived though, when her insurance company refused to pay, and instead authorized cheaper alternatives; alternatives that had already been tried without success.
The desperate patient eventually chose to pay out of pocket for the new, effective medication, at a cost of $600 per month. After a continued back-and-forth, her insurance company finally agreed to cover the costs, and the patient now says her condition is 90 percent improved. In her opinion, she was forced to suffer needlessly. “I think when there is a migraine-specific preventative medicine that is prescribed not just by a neurologist but a migraine specialist,” she told PEW Stateline, “an insurance company shouldn’t have the right to reject it.”
Examples like this can be found in every town and community nationwide. And while this patient had a favorable outcome, many do not. Now though, technology-based eVoucher and denial conversion solutions, including PrimeRx eVoucher and Denial Conversion Services, allow pharmacies to help patients navigate payer obstacles and obtain the medications they need.
References
- “Copayment Adjustment Programs,” National Conference of State Legislators (NCSL), April 4, 2022.
- Dafny, Leemore; Ho, Kate; and Kong, Edward, “How Do Copayment Coupons Affect Branded Drug Prices and Quantities Purchased?,” National Bureau of Economic Research working paper, February 2022.
- “eVoucherRx: Prescription Co-Pay Assistance Program for Pharmacies,” McKesson, accessed September 14, 2022.
- Greenwalt, Luke, “Understanding the Impact of Cost Sharing in Pharma: Cost is a Powerful Control of Patient Behavior,” IQVIA Blog, November 30, 2021.
- Koulianos, Kollet, and Norris, Kerri, “Copay assistance should count as part of patients’ cost sharing for medications,” STATnews, June 30, 2021.
- Ollove, Michael, “Laws to Help Patients Get Pricey Drugs Fall Short, Advocates Say,” Stateline by PEW, June 3, 2021.
- “The Use of Medicines in the U.S. 2022,” The IQVIA Institute, April 2022.
- VanNuys, Karen; Joyce, Geoffrey; and Ribero, Rocio, “Prescription Drug Coupons: A One-Size-Fits-All Policy Approach Doesn’t Fit the Evidence,” Health Affairs, February
16, 2018. - VanNuys, Karen; Joyce, Geoffrey; Ribero, Rocio; and Goldman, Dana, “Prescription Drug Copayment Coupon Landscape,” white paper, University of Southern California
Leonard D. Schaffer Center for Health Policy & Economics, February 7, 2018.
PrimeRx “A Solution For Every Pharmacy”
We are a market leader in the pharmacy software industry with pharmacy management systems installed in pharmacies nationwide.
With almost 30 years of experience, we understand the changing dynamics of the pharmacy system industry better than our competitors, and the critical role of technology in adapting to those changes. Our company motto, “Software without Limits,” is testament to our commitment to continual improvement and innovation. Your pharmacy’s technology system is only as good as its next upgrade. Our customers trust us to provide the technology pharmacy solutions that meet their unique pharmacy software needs. And our customers know they can rely on our superior customer service to provide immediate assistance when needed.

